Subtotal ¥0.00
Explore innovations in pediatric hospital patient identification with durable thermal wristbands enhancing safety accuracy and compliance in children’s care.
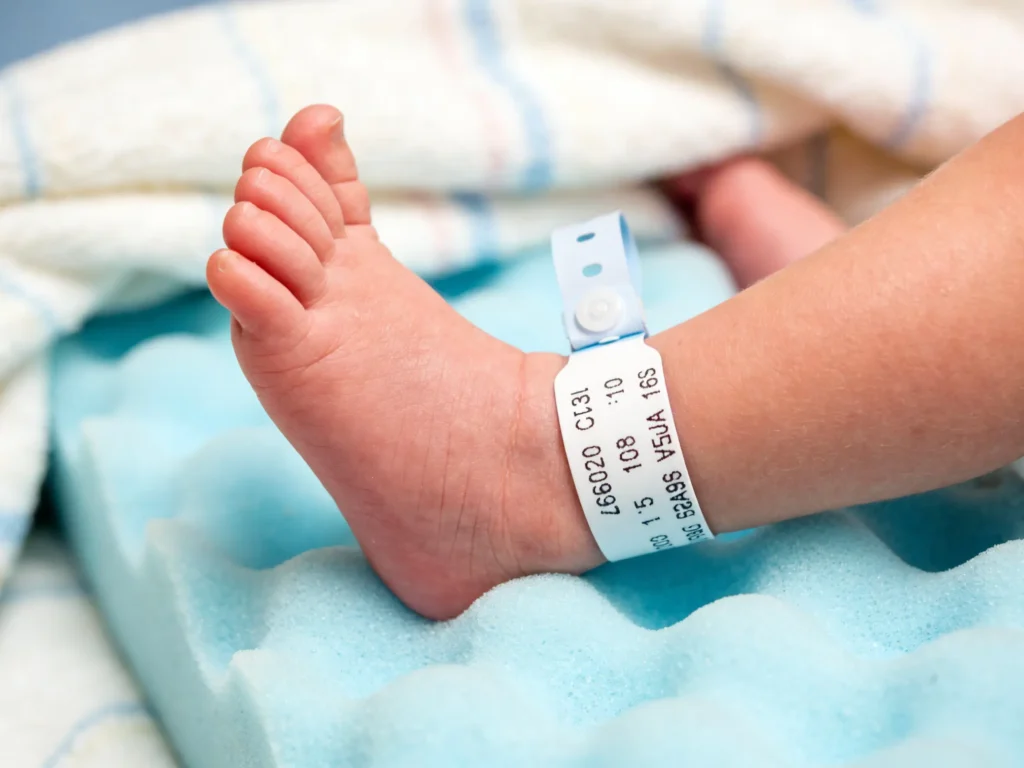
Understanding Patient Identification Challenges in Pediatric Hospitals
Patient identification in pediatric hospitals presents unique challenges that differ significantly from adult care. Non-verbal infants and indistinguishable newborns—especially multiples like twins or triplets—cannot confirm their identities, making reliable identification essential. The patient demographics are fluid, with children growing rapidly and frequently changing rooms or units. Pediatric patients also tend to have longer average stays, increasing the potential for identification errors. Moreover, healthcare providers rely heavily on caregivers for verification and communication, adding complexity to the process.
Common risks related to pediatric hospital patient identification include medication and administration errors, lab specimen mismatches, wrong-site procedures, privacy breaches, financial penalties, and the profound emotional impact on families. These errors can lead to serious harm and diminished trust in the healthcare system.
Regulatory bodies have established clear guidelines to mitigate these risks. The Joint Commission mandates the use of two patient identifiers in all settings, with additional newborn-specific requirements to enhance safety. Organizations like the World Health Organization (WHO) and various children’s hospital associations provide further recommendations tailored to pediatric environments.
Real-world data highlight that neonatal intensive care units (NICUs) and pediatric intensive care units (PICUs) face higher misidentification risks due to critical care intensity and multiple tests or treatments. Integration challenges between electronic health records (EHR) systems and identification tools often impede seamless verification. Notably, family involvement in the verification process is a vital safety net, reinforcing accurate patient identification and fostering collaboration between healthcare teams and caregivers.
Ensuring positive patient identification (PPID) in pediatrics demands systems designed for these unique challenges, prioritizing accuracy, comfort, and family partnership.
Core Components of an Effective Pediatric Patient Identification System
An effective pediatric hospital patient identification system relies on several core components to ensure accuracy and safety. First, it starts with using two unique patient identifiers, usually the child’s full name and date of birth, following Joint Commission patient identifiers guidelines. This helps reduce risks like medication errors or lab specimen mix-ups.
Standardized banding protocols are essential. Wristbands must be designed for fragile skin, offering both durability and comfort, often made with latex-free, antimicrobial materials that resist moisture, sanitizers, and wear. Clear, smudge-resistant barcode printing on these bands ensures reliable scanning, crucial for linking directly to the electronic health record (EHR) and supporting real-time accuracy during medication administration or lab work.
Best practices for pediatric patient ID go beyond wristbands. This includes:
- Bedside barcode scanning before any procedure or medication giving.
- Verbal confirmation of identity by staff with parents or guardians, involving families directly.
- Use of color-coded alerts on wristbands or charts to highlight special conditions.
- Strict protocols during transfers between units to maintain identification integrity.
Additionally, wristbands featuring tamper-evident and antimicrobial properties help maintain band integrity throughout longer stays common in pediatrics. These features prevent accidental or intentional removal and reduce infection risks, supporting a safer environment for vulnerable newborns and infants.
Together, these elements form the backbone of a pediatric patient identification system tailored for children’s unique needs—ensuring every child in the hospital is identified correctly and safely at all times.
Innovations Transforming Patient Identification in Children’s Hospitals
Pediatric hospital patient identification has come a long way from simple handwritten tags to advanced barcode-enabled systems. Today, many children’s hospitals use PPID (Positive Patient Identification) that links wristbands directly to medications, lab tests, and orders. This real-time connection helps reduce errors right at the point of care.
RFID and biometric integrations are also making waves. RFID wristbands enable contactless scanning, speeding up processes without compromising accuracy. New tech like facial recognition and digital footprints offer even more precise verification, reducing risks like duplicate records.
Comfort is key in pediatric ID bands. Designers focus on pediatric-sized and infant-specific wristbands that lessen skin irritation but still perform well under barcode scanners. This means less hassle for kids and families.
Collaboration between hospitals, manufacturers, and tech experts is improving wristband ergonomics and visibility. These redesigns make it easier for staff to check IDs securely and quickly.
Thermal printing technology is a standout innovation, producing high-quality, smudge-proof barcodes on-demand. This flexibility suits the fast-changing needs of pediatric care, ensuring wristbands stay readable and reliable throughout longer hospital stays.
In , innovations like barcode scanning children’s hospitals, RFID wristbands in pediatric care, and AI tools are transforming patient ID systems. These advances improve safety, comfort, and workflow efficiency – essential for the unique demands in children’s hospitals.
Why Thermal Wristbands Excel in Pediatric Identification Systems
Thermal wristbands are a great fit for pediatric hospital patient identification. Here’s why they stand out:
| Feature | Benefit for Pediatrics | Details |
|---|---|---|
| Technical Advantages | Smudge-resistant, clear barcodes on curved small wristbands | High-contrast printing ensures reliable barcode scanning, even on tiny infant wrists. |
| Durability and Safety | Resistant to sanitizers and fluids; latex-free, soft materials | Keeps bands safe and comfortable against sensitive skin; multiple closure types prevent accidental loss. |
| Workflow Benefits | Fast on-site printing reduces errors from pre-printed bands | Quick printing supports real-time updates and seamless EHR & PPID system integration. |
| Proven Practice | Favored in children’s hospitals for long stays and accuracy | Improves medication administration safety and reduces specimen labeling mistakes. |
LinkWin thermal wristbands lead the pack. They’re designed for pediatric comfort and include antimicrobial options to fight infection risks. Their superior print quality ensures barcodes stay crisp, supporting positive patient identification (PPID) in pediatrics.
Overall, thermal wristbands deliver reliable, safe, and efficient pediatric ID solutions — helping hospitals reduce errors and secure patient safety with ease.
Implementing an Innovative Pediatric Patient Identification System: Step-by-Step
Introducing a new patient identification system in a children’s hospital isn’t just about technology—it’s about improving safety and trust. Here’s a simple guide to get it right.
1. Assessment Phase: Know Where You Stand
- Audit current practices: Look closely at how you currently identify pediatric patients. Spot weak points where errors like misidentification or labeling mistakes happen.
- Engage the whole team: Include multidisciplinary experts—nurses, doctors, IT staff, and family advisors. Family involvement is key since parents often help verify identity.
- Identify pain points: Pin down areas like wristband discomfort, barcode scanning failures, or EHR integration issues.
2. Technology Selection: Choose What Fits Pediatric Needs
- Pediatric sizing: Pick wristbands designed for tiny wrists, especially newborns and infants, to avoid skin irritation.
- Barcode symbology: Ensure barcodes are clear, high-contrast, and easy to scan, supporting Positive Patient Identification (PPID) efforts.
- System integration: The ID system should link smoothly with BCMA (Bar Code Medication Administration), lab labeling, and electronic records.
- Cost of ownership: Consider upfront costs and ongoing expenses like supplies and tech support.
3. Training and Change Management: Build Confidence and Compliance
- Staff education: Everyone must understand how to apply wristbands, scan barcodes, and involve families in verification.
- Family engagement: Teach parents how they can help prevent errors by verifying wristbands during care.
- Monitor compliance: Use regular audits and feedback to ensure staff follow protocols.
4. Systems Integration: Make It a Connected Process
- Link wristbands directly to medication orders, lab tests, and patient records in the EHR.
- This closed-loop system reduces risks like wrong-site procedures or lab specimen mismatches.
5. Measuring Success: Track Impact Clearly
- Error reduction: Monitor drops in misidentification cases.
- Band compliance: Ensure wristbands are worn consistently and correctly.
- Scan rates: Track how often wristbands are scanned before procedures.
- Satisfaction surveys: Collect feedback from staff and families on system usability and comfort.
6. Overcoming Barriers: Address Challenges Head-On
- Resistance: Some staff or families may hesitate; clear communication helps.
- Budget limits: Focus on long-term savings from fewer errors and better care.
- Equity: Ensure equal access for all patients, regardless of background or insurance.
By following these steps, children’s hospitals can implement a reliable, innovative patient identification system that supports safety, comfort, and accurate care delivery across pediatric settings.
The Human Impact: Enhancing Safety, Trust, and Outcomes
Using an innovative pediatric hospital patient identification system has a real, positive effect on patients and families. When identification is clear and reliable, anxiety drops because parents feel confident their child is safe. Clear communication between caregivers and families reduces mistakes in medication and procedures, preventing errors that can be harmful or even life-threatening.
Clinically, hospitals see fewer adverse events and smoother workflows. Staff spend less time double-checking and more time focusing on care. Better interoperability between electronic health records (EHR) and bedside systems means information flows seamlessly, supporting value-based care goals. This boosts overall patient safety and hospital efficiency.
Real-world cases show that using advanced Positive Patient Identification (PPID) wristbands, especially those with barcode scanning, cuts down mislabeling and improves compliance with safety protocols. For example, NICUs and PICUs have reported significant drops in specimen mismatches and medication errors after adopting these systems.
Looking ahead, the future of pediatric patient ID lies in hybrid systems. Combining thermal printable hospital wristbands with biometric tools or Internet of Things (IoT) technology promises even greater precision. This blend ensures every newborn or child, even those who can’t speak or move much, is identified correctly every time — building stronger trust with families and improving outcomes worldwide.

